All posts by DentMistry
History, clinical examination and treatment planning
History
Biodata
- Date
- File number
- Full name
- Age/date of birth
- Gender
- Contact
- Physical address
- Occupation
- Name of guardian/parent – for children
- Source of referral (if referred)
Presenting complaint
In patients own words, what is the problem
History of presenting complaint
- S – Site
- O – Onset
- C – Character (throbbing, continuous, dull, acute, sharp)
- R – Radiation (to head)
- A – Associated symptoms (fever, discharge)
- T – Timing (day or night, after eating)
- E – Exacerbating factors (hot/cold food), Alleviating factors (Pain medications)
- S – Scale (scale of 1-10, rate the pain)
Previous treatments concerning the presenting complaint
Past dental history
- Index visit or
- Previous dental treatments done
- What they were
- When
- Where
- If extraction done – any complications
- Tolerance to LA
Dental habits
- How many times do they brush their teeth
- How do they brush
- Which toothpaste
- How often they change their brush
- Any interdental cleaning methods used – floss, toothpicks
- Abnormal habits eg. mouth breathing, lip sucking
Past medical history
- History of chronic illness:
- CHD/CVS, infective endocarditis
- Respiratory – asthma, bronchitis
- GIT – peptic ulcers, diarrhea, vomiting, jaundice, hepatitis, gastritis
- Diabetes
- CNS disorders
- Bleeding disorders – hemophilia, anticoagulant therapy
- Infectious diseases – TB, HIV, Herpes
- On any medications – NSAID, corticosteroids, anticoagulants, anticonvulsants
- Previous hospital admission – When, where, why, treatment provided
- Food or drug allergy
Obs and gyn history for females
- Last menstruation date and regularity
- Pregnancy status
- Type of contraceptives used
Family social history
- Alcohol – amount and frequency
- Smoking – amount and frequency
- Drugs
- Family status – parents, siblings, chronic illness in family
- Martial status and children
- Water source – borehole or city council
For pediatric and orthopedic patients
Birth history:
Prenatal:
- Health and nutritional status of mother during pregnancy
- Complications during pregnancy:
- Infections – rubella, TB, syphilis, UTI
- Pre-eclampsia
- Hypertension
- Diabetes
- Antepartum bleeding
- Drugs
- X-ray
- Rh incompatibility may result in erythroblastosis fetalis – leading to green blue discoloration of dentition. Picture
Natal:
- Full term or premature
- Mode of delivery – Normal/C-section and why?
- Did the baby cry on birth
- Birth weight
- Breast fed or formula milk given
Postnatal:
- Vaccinated
- Developmental history
- Nocturnal feedings/sweetened milk – predisposes to early childhood caries (read more)
- Brushing habits – frequency, by who, supervised?
Habits
- Finger sucking/thumb sucking
- tongue thrusting
- Mouth breathing
- Nail biting – check nails
Diet chart
- 24 hour diet chart
- 7 day diet chart (as investigation)
Family social history
- Name of school
- Class
- Performance in school
- Social or antisocial
- Occupation of parents
- Family history
- Water source
Clinical examination
General examination
- Anxious or calm
- Build, nourishment – well, poor
- Posture
Vital signs:
- Temperature
- Pulse rate
- Respiratory rate
- Blood pressure
NB: Also measure weight and height for children – to calculate BMI and dosage of LA and drugs
Extra oral examination
- Palpate submental, submandibular and neck lymph nodes
- Facial symmetry – any swellings or asymmetry
- Facial profile
- Scars
- Eyes – jaundice (look down), pallor (look up)
- TMJ movements – clicking or popping sounds, pain, path of closure
- Lips competency
- Hands – examine nails, finger clubbing, cyanosis
Remember it as: J A C C L O W D (Jaundice, anemia, clubbing, cyanosis, lymphadenopathy, oedema, wasting, dehydration)
Intraoral examination
- Oral hygiene status
- Type of dentition: primary, mixed, permanent
Soft tissue examination:
- Gingiva – shape, size, color, bleeding, ulceration, growths, pockets, recession
- Plaque and gingival score
- Buccal mucosa – color, texture, ulcer, growth, sinus
- Floor of mouth – swellings, ulcer
- Tongue – size, movements, plaque
- Palate – normal, high vault, clefts
- Tonsils – normal, swollen
- Frenal attachments – normal, higher
Hard tissue examination:
- According to quadrants
- Teeth present
- Teeth missing
- DMF
- Palpate, percuss
- Check interproximal caries with floss
- Wear (attrition, abrasion, erosion)
- Discoloration
- Malformation
- Mobility – Millers classification 1950
- 0 = No detectable mobility
- 1 = Distinguishable mobility
- 2 = Horizontal movement > 1mm
- 3 = Horizontal and vertical movement > 1mm
- Orthodontic assessment
- Fluorosis – TF score for every tooth
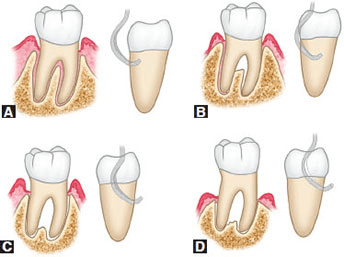
Tooth fracture classification
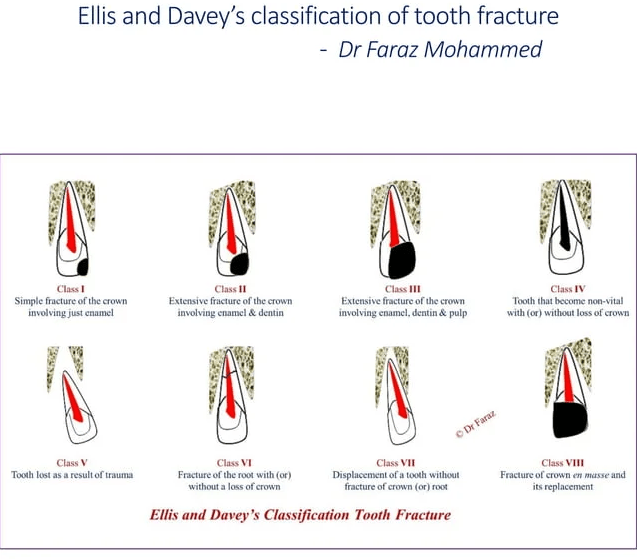
Periodontal assessment
Gingiva:
- Color: Pink, physiologic pigmentation, red, cyanotic
- Size: Mild, moderate, severe inflammed
- Shape: Scalloped, rounded, col – if space between 2 teeth
- Consistency: Firm, flabby
- Texture: Stippling on attached gingiva
Oral hygiene:
- Calculus – presence of supra or subgingival calculus
- Plaque seen with naked eye
Gingival index by Loe and Silness 1963:
- Facial and lingual surface of index teeth: 16, 11, 24 and 36, 31, 44
- Rate:
- 0 = Normal
- 1 = minimal inflammation, erythema, no bleeding
- 2 = Bleed on probing
- 3 = Spontaneous bleeding
- Find mean score
- GI score:
- 0-1 = Mild
- 1-2 = Moderate
- 2-3 = Severe
Periodontal index by Turesky et al modified Quigley Hein 1970:
Index teeth and disclosing tablet
- 0 = No plaque
- 1 = Flecks at cervical margin
- 2 = Thin continuous band at cervical margin
- 3 = Band wider than 1mm, < 1/3 of crown
- 4 = Plaque < 2/3 of crown
- 5 = Plaque > 2/3 of crown
Furcation involvement – Glickman classification 1953
- Grade 1 – Incipient, pocket formation into furcation fluting, interradicular bone intact
- Grade 2 – Moderate loss of interradicular bone but not through and through
- Grade 3 – Probe goes through and through, orifice occluded by gingival tissue
- Grade 4 – Exposed furcation
Periodontal charting:
- Draw continuous line of free gingival margin – facial and lingual
- Draw interrupted line indicating bone level on facial side
- Record 6 point pocket depth
- Record tooth mobility
- Record missing teeth (X), open contacts(//) and how many mm, overhang restorations (V)
- Calculate clinical attachment loss (CAL): Gingival recession + pocket depth
- 1-2mm = Mild
- 3-4mm = Moderate
- > 5mm = Severe
- Localized: < 30% of sites
- Generalized: > 30% of sites
Orthodontic assessment
- A-P: Molar, canine, incisor relationship – Class I, II, III
- Vertical: Open bite, overbite – deep or open
- Transverse:
- Crossbite anterior or posterior
- Midlines
- Crowding or spacing
- Rotation or displacement
- Proclination
- Upper and lower arch form – Normal, V shape, square shape
Investigations
- Radiological – describing a x-ray:
- Name and age of patient
- Date when the x-ray was taken
- Quality
- Teeth present
- Dental age and why
- Radiolucent/radiopaque lesions
- Microbiological
- Histopathological
- Study model
- Diet chart
- Plaque score
- BMI
Diagnosis
- Summarize findings: eg. A 5 year old African male with early childhood caries, dentoalveolar abscess secondary to extensive decay on 55, irreversible pulpitis 85 and 75, and occlusal caries on 54, 64, 84, 74
- For periodontal diagnosis: Severity – extent – diagnosis, eg:
- Mild – localized – chronic periodontitis
- Moderate – generalized – plaque induced gingivitis secondary to orthodontic treatment and mouth breathing
Prognosis for periodontology
1. Excellent prognosis:
- No bone loss
- Excellent gingival condition
- Good patient co-operation
- No systemic/environmental factors
2. Good prognosis:
- Adequate remaining bone support
- Adequate control of etiologic factors and maintainable dentition
- Adequate patient co-operation
- No systemic/environmental factors or well controlled
3. Fair prognosis:
- Less than adequate bone support
- Some tooth mobility
- Grade 1 furcation
- Adequate maintenance possible
- Acceptable patient co-operation
- Presence of limited systemic/environmental factors
4. Poor prognosis:
- Moderate-advanced bone loss
- Tooth mobility
- Grade 1 or 2 furcation involvement
- Doubtful patient co-operation
- Presence of systemic/environmental factors
5. Questionable prognosis:
- Advanced bone loss
- Tooth mobility
- Grade 2 or 3 furcation involvement
- Inaccessible areas
- Systemic/environmental factors
6. Hopeless prognosis:
- Advanced bone loss
- Extraction indicated
- Non maintainable areas
- Uncontrolled systemic/environmental factors
NB: Factors affecting prognosis:
- Diagnosis: Disease severity, plaque and calculus
- Systemic factors: DM, puberty, genetic
- Occlusal factors
- Prosthetic and restorative factors: Caries, teeth vitality, abutment selection, subgingival restorations, fixed or removable prosthesis
- Patient factors: Compliance, co-operation, attitude
- Environmental factors: Smoking, alcohol. bruxism
Treatment objectives
- To control infection and relieve pain and discomfort
- To modify attitude to dental care, and behavior to dental treatment
- To improve oral hygiene
- To restore integrity and function of the dentition
- To achieve cariostasis
- To improve esthetics and correct malocclusion
- To maintain a healthy oral cavity
- Diet planning
Treatment planning
- Oral hygiene instruction (OHI)
- Emergency phase: Systemic diseases, infections
- Etiological phase: Plaque and calculus
- Restorative phase: Filling, RCT, Prosthetic replacement
- Maintenance phase: Recall and review
Periodontal treatment planning
- Preliminary phase: Systemic disease, infections, OHI
- Etiological phase: FMS, root planing, fluoride treatment, cavity prep and filling
- Surgical phase: Disimpaction, gingivectomy, implants, open flap debridement, GTR, furcationplasty
- Restorative phase: Crown, bridge, crown for implant
- Supportive periodontal therapy/maintenance phase: Review after 2 weeks
- High risk – recall every 3 months
- Moderate risk – recall every 6 months
- Low risk – recall every year
Pediatric treatment planning
- Systemic phase – Stabilize chronic illness before dental treatment
- Emergency phase – Antimicrobials
- Preventive phase – OHI, behavior management, fluoride application, diet counselling, pit and fissure sealants
- Preparatory phase – Oral prophylaxis, caries control if multiple lesions, preventive orthodontic consultation
- Corrective phase – Restorations, prosthetic replacement, extractions, Interceptive orthodontic consultation
- Maintenance phase – Recall and review, 3-6 months
- Significance of oral prophylaxis:
- Introduction to dental environment/behavior management
- Oral hygiene education
- Uncover carious lesion covered in plaque
- Healthy gingiva
Orthodontic History, Examination, Investigation, Treatment Planning and Cephalometric Analysis
History:
- Biodata
- Presenting complain
- HPC
- PDH
- Dental habits
- PMH
- FSH
- Birth history
- Abnormal habits
Clinical examination:
General examination
Extraoral examination:
- JACCLOWD
- TMJ movements – clicking or popping sounds, pain, path of closure
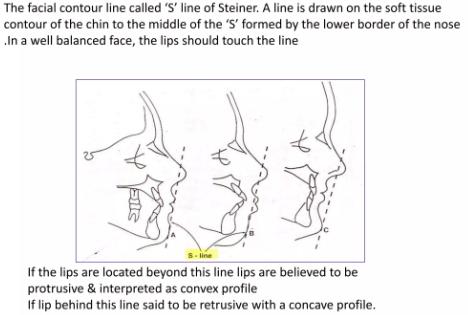
- Facial profile
- Facial symmetry
- Lip competency
- Incisor showing on smiling – Normally 2-4mm
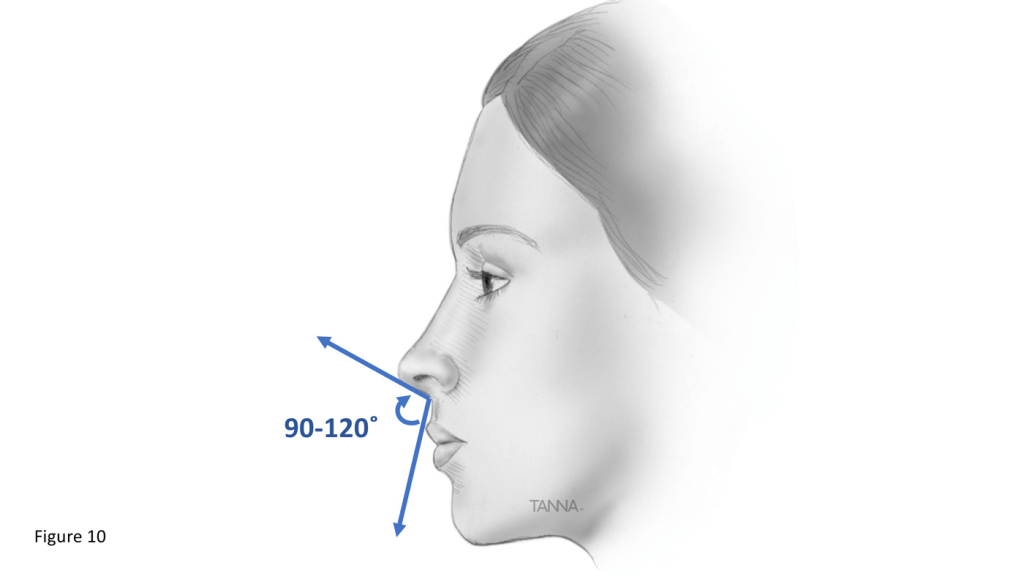
- Nasolabial angle and lip protrusion:
- Between upper lip and base of nose
- Normal 90° – 110°
- Convex – Class II, retrusive mandible
- Concave – Class III, protrusive mandible
- Becomes retrusive and obtuse angle with age
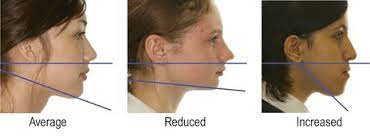
- Vertical facial relationship – Angle of lower border of mandible to cranium
- Use occipital region to draw imaginary line
- Average
- Reduced – Short face syndrome: Deep bite, overlapped lips
- Increased – Long face syndrome: Anterior open bite, incompetent lips
Intraoral examination:
- Oral hygiene status
- Type of dentition: primary, mixed, permanent
- Soft tissue and hard tissue examination
- Dental arches:
- Crowding: mild, moderate, severe
- Spacing
- Tooth rotations: mesioversion, distoversion lingoversion, buccoversion, labioversion)
- Tooth displacement
- Ugly duckling stage
Orthodontic examination:
- Anterior – posterior plane: Molar, canine, incisor relationship – Class I, II, III
- Molar malocclusions: Maxillary 6 MB cusp and mandibular 6 buccal groove.
- Angles class I: 7 types:
- 1. Maxillary teeth crowded
- 2. Anterior teeth proclined
- 3. Anterior crossbite
- 4. Posterior crossbite
- 5. Permanent molars drifted mesially
- 6. Diastema
- 7. Deep overbite
- Angles class II:
- Division I: Incisors proclined
- Division II: Incisors retroclined
- Subdivision: if right or left unilateral Angles class II
- Angles class III:
- Type 1: Edge to edge bite
- Type 2: Normal overbite
- Type 3: Anterior cross bite
- Pseudo class III malocclusion: Mandible moves forward
- Angles class I: 7 types:
- Molar malocclusions: Maxillary 6 MB cusp and mandibular 6 buccal groove.
- Vertical plane:
- Overbite: Normal 20-40%. <20% = reduced overbite, >40% = deep bite
- Open bite
- Anterior crossbite/ reverse overjet
- Transverse plane:
- Midline
- Crossbite
- Scissor bite
Investigation
- OPG, study model, photograph, lateral cephalogram, CT scan
OPG:
- Name and age of patient
- Date when the x-ray was taken
- Quality
- Teeth present
- Dental age, development of crown and roots, root completion 2-3 years after eruption
- Radiolucent/radiopaque lesions
Study model analysis: Note date of impression, patient name, D.O.B, file number
a) Interarch analysis:
- A-P, transverse, vertical plane
- Use dividers to measure
b) Intra arch analysis: Maxillary and mandibular
- Shape (U, V)
- Arch symmetry (position of teeth, missing teeth)
- Palate vault
- Number of teeth present, or eupting
- Individual tooth malformation, malposition, or rotation
c) Space analysis:
- Arch parameter (X) = Measure arch from 5 to 5, distal surface
- Tooth material (Y)= Width of each tooth. Angles lines of occlusion:
- Maxillary – use central fossa and cingulum (in anterior teeth)
- Mandible – use buccal cusp tips and incisal edges
- Difference between arch parameter and tooth material:
- X – Y = Positive (spacing), Negative (crowding)
- ≤ 4mm = Mild crowding
- 5-8 mm = Moderate crowding
- > 9mm = Severe crowding
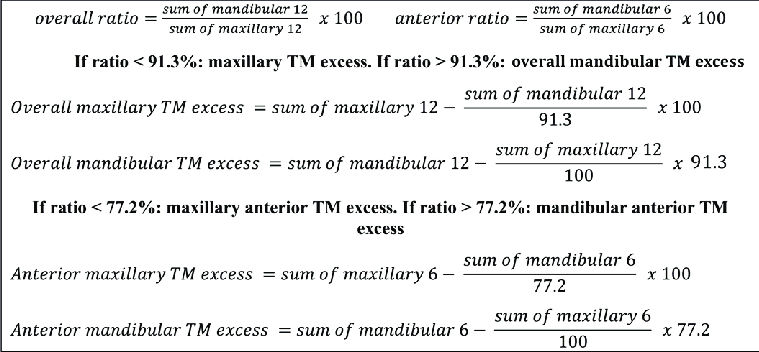
d) Bolton’s analysis: Maxillary and mandibular relationship for overbite/overjet
- Sum of mesiodistal width of 12 teeth: CI, LI, C, PM, PM, M1 on both sides
Sum of mandibular 12/Sum of maxillary 12 X 100 = 91.3% ± 1.91 (ie. range: 89.39-93.21)
- < 91.3% = Maxillary teeth in excess
- >91.3% = Mandibular teeth in excess
e) Anterior ratio: Maxillary and mandibular relationship for overbite/overjet
- Sum of mesiodistal width of 6 teeth: CI, LI, C on both sides
Sum of mandibular 6/Sum of maxillary 6 X 100 = 77.2% ± 1.65 (ie. range: 75.55-78.85)
- < 77.2% = Anterior maxillary teeth in excess
- >77.2% = Anterior mandibular teeth in excess
NB: Bolton’s analysis and anterior ratio cannot work if required teeth are missing

Photographs: Smile and profile analysis, record keeping
Lateral cephalogram analysis
Mixed dentition analysis using study models:
a) Radiograph/Huckaba analysis:
True width of 1st molar/Apparent width of 1st molar = True width of unerupted PM/Apparent width of unerupted PM
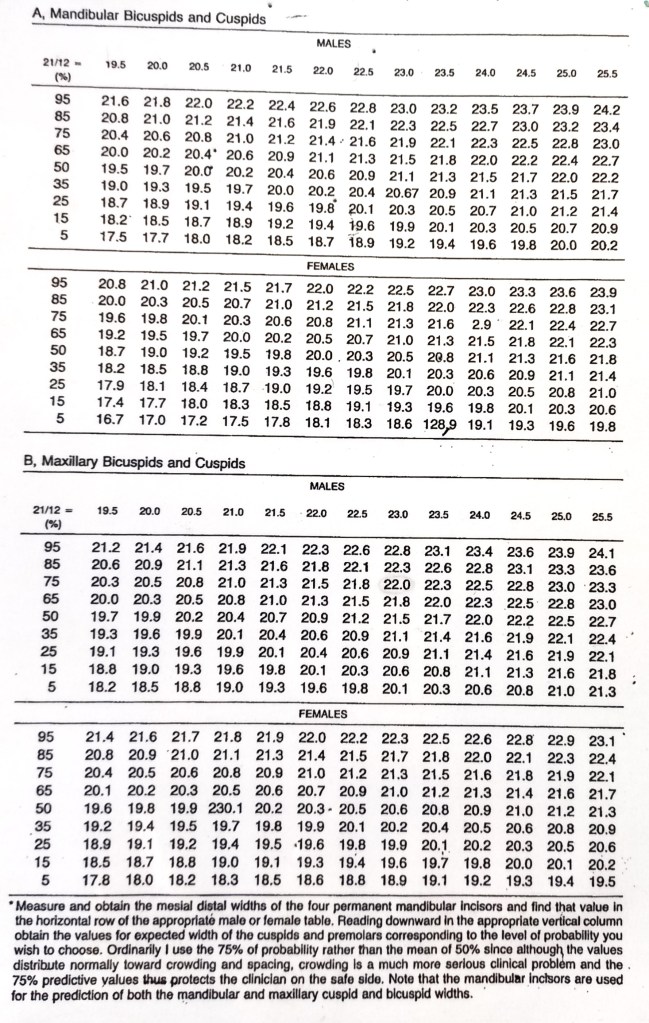
b) Moyer’s prediction table:
- Use sum of mandibular 4 incisors to predict mesiodistal width of permanent canine and premolars
- 75 percentile usually used
c) Tanaka and Johnston:
- Estimated mesiodistal width of canine and premolar of one quadrant = 1/2 of the mesiodistal width of mandibular 4 incisors + 10.5mm (for mandible) or 11mm (for maxilla)
d) Nance – Arch perimeter analysis:
- Mesiodistal width of erupted permanent teeth and from IOPA of unerupted teeth
Diagnosis
- List name, age and gender
- Write problem list in priority
- Eg. Angles class I malocclusion with an anterior open bite extending from 15/45 to 25/35, with an overjet of 6mm and tongue thrusting habit
Treatment plan
- List treatment objectives according to PC and priority
- List treatment plan
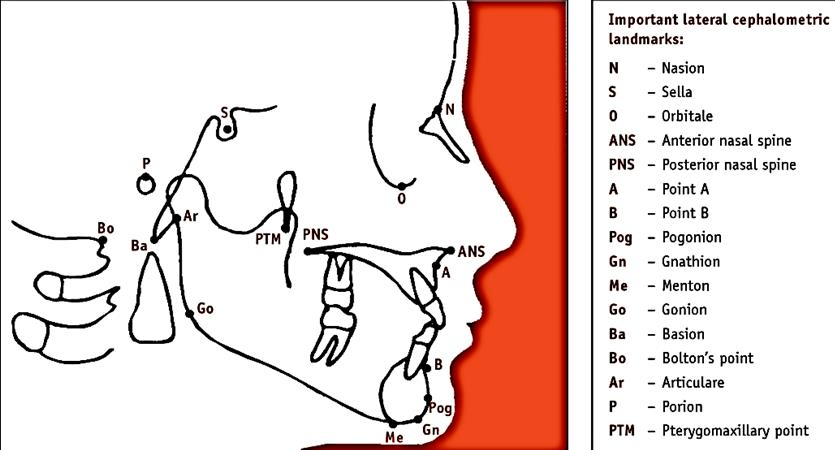
Cephalometric analysis
- S – Sella turcica – center of pituitary fossa
- N – Most anterior point of frontal and nasal bone junction
- A – Inner most point between ANS and incisor
- B – Inner most point between mandible and incisor
- Pog – Anterior most point of mandible
- Gn – Most anterior inferior point of bony chin
- Go – Point where posterior border of ramus and lower border of mandible bisect
- Porion – External auditory meatus upper contour midpoint
- Orbitale – Inferior margin of orbit – lowest point
- Frankfort plane (FH) – Porion to orbitale
- Occlusal plane – Use molars and premolars
- Mandibular plane – Gn to Go
Steiner’s analysis
Skeletal analysis:
1. SNA angle: 82° ± 2
- Ant-post position of maxilla with cranial base
- Increased angle = Prognathic maxilla
2. SNB angle: 80° ± 2
- Ant-post position of mandible with cranial base
3. Angle ANB: 3 ± 1
- Difference between SNA and SNB – magnitude of skeletal jaw discrepancy
- Factors affecting:
- Vertical height of face
- Abnormal position of nasion
- Increased angle = Class II
- Decreased angle = Class III
4. Mandibular plane angle: 32° ± 4
- Steepness of mandibular plane to cranial base
- Increased angle = Vertical growth
- Decreased angle = Horizontal growth
5. Occlusal plane angle: 17° ± 4
- Determine relationship of teeth in occlusion with cranial base
- Increased angle = Skeletal open bite
- Decreased angle = Skeletal deep bite
Dental analysis:
1. UI – NA angle and distance: 22°, 4mm
- > 4mm or increased angle = Protrusion eg. class II division 1
- < 4mm or decreased angle = Retrusion eg. class II division 2
2. LI – NB angle and distance: 25°, 4mm
- > 4mm or increased angle = Protrusion eg. class II division 1
- < 4mm or decreased angle = Retrusion eg. class II division 2/ class III
3. Interincisal angle: 130°-131°
- Increased angle = Class II division 2
- Decreased angle = Class II division 1
4. Lower incisor to chin (Holdaway ratio)
Soft tissue analysis:
Langerhans cell histiocytosis
Formerly known as histiocytosis x (eosinophilic granuloma, hand-schuller-christian disease, letterer-siwe disease)
- Due to proliferation of abnormal histiocytes (subtypes of WBC)
Clinical: Short stature, diabetes insipidus, neurosensory deafness and tooth mobility
Radiology: Osteolysis causing ’floating teeth’ in multiple quadrants
Histology:
- Diffuse infiltration of large, pale staining mononuclear cells with indistinct cytoplasmic
borders rounded/bean shaped nuclei - Birbeck granules: rod shaped cytoplasmic structures characteristic to Langerhans cells (s100 positive)
Management: Curettage of accessible bone lesions
Scurvy
- ↓ Ascorbic acid (vit C)
Physiology: Vit C is required for redox reactions:
- Hydroxylation of praline in collagen formation
- Hydroxylation of dopamine to noradrenaline
Clinical: Scurvy
- Haemorrhagic diatheses
- Skin rash
- Delayed wound healing
- Anaemia
- Scorbutic rosary – mineralization of costochondral cartilages due to deranged formation
of osteoid - Generalized gingival enlargement
Histology: Hemorrhagic gingival enlargement with minimal fibrosis
Management: Replacement therapy
Renal osteodystrophy and rickets
- Skeletal abnormalities due to chronic renal failure
- Kidneys are vital of vit D metabolism, and phosphate secretion – when disturbed results in:
- Osteomalacia (or rickets)
- Secondary hyperparathyroidism
- Metastatic calcification
- Osteoporosis
Rickets:
Deficiency of vitamin D during bone development (infancy)
- Essential for absorption and metabolism of calcium and phosphate
- Deficiency leads to:
- Defect in bone matrix mineralization and skeletal development
- Defective absorption of calcium and phosphate
- Chronic renal disease: renal rickets
Etiology:
- 1. Vitamin D deficiency
- Reduced endogenous synthesis due to lack of exposure to the sun
- Dietary deficiency (fish, eggs, butter, milk)
- Malabsorption and metabolism failures due to liver disease, pancreatic insufficiency, kidney
- 2. Abnormal metabolism of vitamin D:
- Chronic renal failure
- Vitamin D resistant rickets
- Anticonvulsant osteopathy
- 3. Phosphate depletion: antacids contain al(oh)3 which bind phosphate, excess renal secretion of po4
- Fanconi syndrome
- X linked hypophosphatemic rickets
- 4. Renal tubular acidosis
Physiology:
- Vit D is essential for intestinal absorption of Ca++ and po4
- Co-factor in mobilization of Ca++ from bone
- Stimulates PTH dependent re-absorption of Ca++ by the distal renal tubules
Clinical:
- Craniotabes – unossified areas of cranium
- Rachitic rosary – overgrowth of costochondral cartilage
- Pigeon chest deformity
- Lordosis
- Knock knees/ bow legs
- Enlarged epiphyses
- Osteomalacia
- Hypocalcaemic tetany
- Dental:
- Multiple spontaneous periapical abscess in 1ry & 2ry dentition
- Enlarged pulp chambers
- Thin easily abraded enamel
- Marked interglobular dentine
Histology: ↑ Osteoid matrix in bones
Lab:
- Normal or ↓ ca++
- ↓ po4
- ↓ vit D metabolites
- ↑ alkaline phosphatase
Management: Replacement therapy
Osteoporosis
- Quantitative reduction of normal bone → risk of fractures, pain, bone deformity
Etiology/classification:
1. Primary – Osteopenia without an underlying disease or medication
- Idiopathic type – rarely, in young pt
- Involutional type – postmenopausal women and geriatric patient
Contributing factors:
- Race (more in caucasians and asians)
- Gender: F > M.
- Reduced physical activity (convalescence and old age)
- Oestrogen, calcitonin and androgen deficiencies
- Malnutrition states
- Hyperparathyroidism
- Vitamin d deficiency
2. Secondary – due to:
A. Endrocrine disorders:
- Hypogonadism
- Hyperparathyroidism
- Pituitary tumours
- Type 1 diabetes
- Addison disease
- Thyrotoxicosis
B. Neoplasia: multiple myeloma, carcinomatosis
C. Git problems: malnutrition, malabsorption, hepatic insufficiency, vit c & d deficiency
D. Medication: corticosteroids, anticonvulsants, heparin, alcohol
E. Miscellaneous: immobilization, anemias, pulmonary disease
Radiology: Enlargement of the medullary cavity + thinning of cortex
Histology:
- Active type – ↑ bone turnover – by osteoblastic and osteoclastic activity with new osteoid formation
- Inactive osteoporosis – almost normal bone structure
Lab: ↑ serum phosphatase
Management: Hormone replacement therapy, manage other underlying causes
Osteitis deformans – Paget’s disease
Abnormal and anarchic resorption and deposition, resulting in distortion and weakening of the affected bones
Epidemiology: M > F, patients over 50 years, Max > Mand (2:1)
Etiology:
- Slow paramyxovirus infection
- Vascular disorder
- AD
Pathology:
- Fast, irregular, exaggerated bone remodelling
- Thick bones without localized swelling
- Early phase – resorption
- Late stage – sclerosis
- Patchy appearance due to areas of resorption and sclerosis adjacent to each other
Clinical:
- Simian stance due to weakening of weight bearing bones,
- Lion-like facial deformity (bilat symmetrical bone enlargement)
- Pain on involved bones
- Hypercementosis
- Neurological symptoms due to narrowing of foramina:
− Headache
− Vertigo
− Visual disturbance
− Auditory disturbance
Complication: (0.9 – 13%): progression to osteosarcoma
Histology:
- Initial osteolytic – osteoclastic bone resorption
- Mixed osteolytic/osteoblastic stage -mosaic pattern of reversal lines (osteoid seams)
- Quiescent osteosclerotic stage – dense bone with remnants of mosaic patterns
X-ray:
- “Cotton wool” appearance of confluent radio-opacities
- Thickening of bone
- Irregular areas of sclerosis and resorption
- Loss of normal trabeculation
Lab:
- ↑alkaline phosphatase
- Normal calcium and phosphorus levels
- ↑ urinary hydroxyproline
Management: Seldom fatal
- Surgical debulking + calcitonin (PTH antagonist) + sodium phosphatase (retards bone resorption)
Infantile cortical hyperostosis – Caffey’s disease
- Children under 1 year of age
Etiology: AD or sporadic form – osseous growth spurt during development.
Common sites:
- Mandible
- Clavicle
- Scapula
- Frontal bone
- Ulna
Radiology: Mandibular enlargement, cortical redundancy
Lab:
- Anemia
- Leukocytosis
- ↑ ESR
- ↑Serum alkaline phosphatase.
- Monocytosis
Management: Symptomatic
Hypothyroidism
- ↓ Thyroid hormone
Etiology:
- Congenital defects of the thyroid
- Iodine deficient goiter
- Autoimmune (Hashimoto’s) thyroiditis
- Diseases of the pituitary (↓TSH)
- Hypothalamus (↓ thyrotropin releasing hormone TRH)
- Radiation injuries
- Surgical ablation
- Drugs (lithium, iodides)
- Idiopathic causes
Clinical:
- Delayed mental, skeletal, dental and sexual development
- Blood: microcytic, hypochromic anemia – fatigue and lethargy
- Dermal: dry and scaly skin, facial oedema.
Management: Gradual replacement therapy + synthetic and natural thyroid hormone preparations.