The intraembryonic mesoderm differentiates into:
- Paraaxial mesoderm
- Intermediate mesoderm
- Lateral plate mesoderm
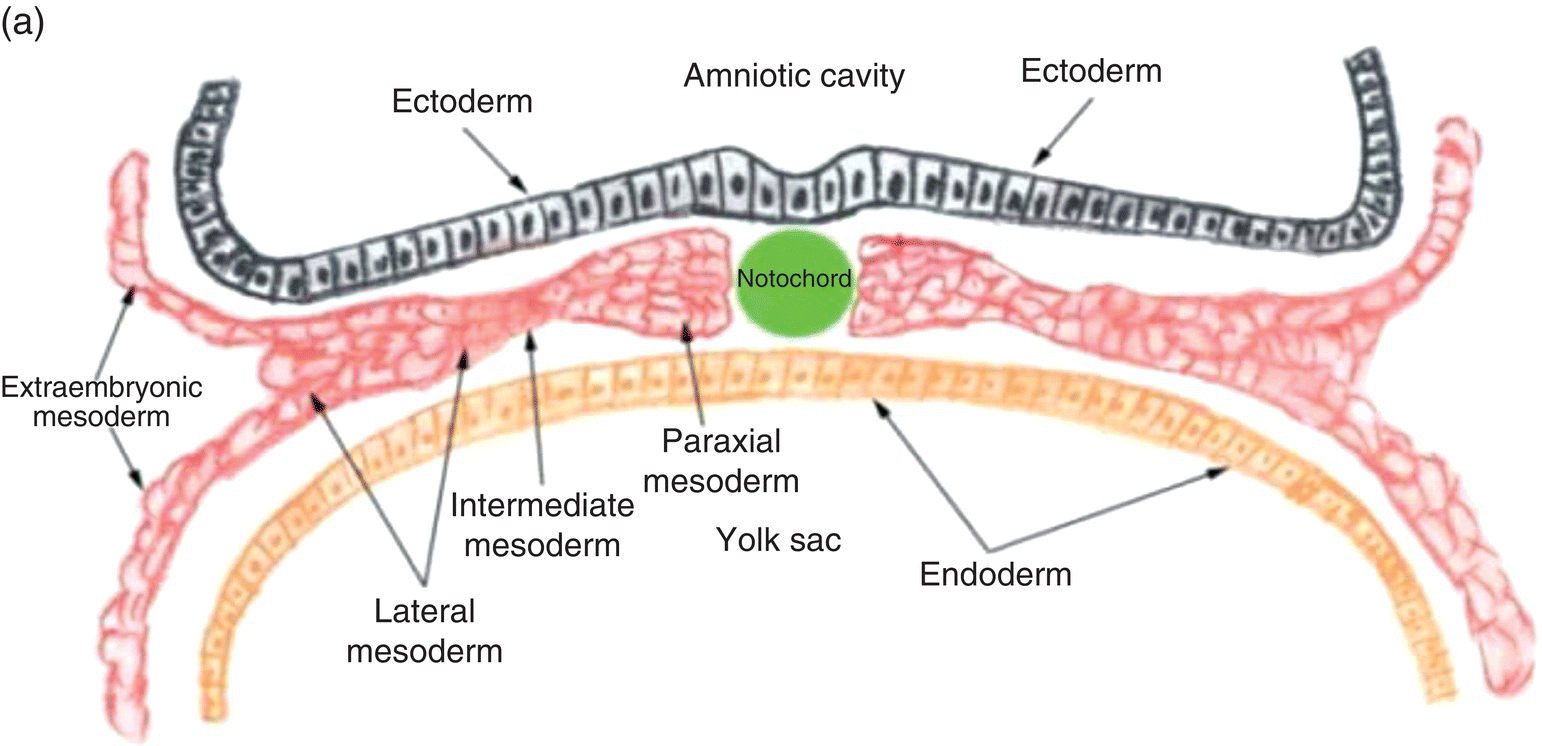
Paraaxial mesoderm
Transverse grooves appear dividing it into somites, from cranial to caudal end.
42 to 44 somites form;
- 4 occipital
- 8 cervical
- 12 thoracic
- 5 lumbar
- 5 sacral
- 8 – 10 coccygeal
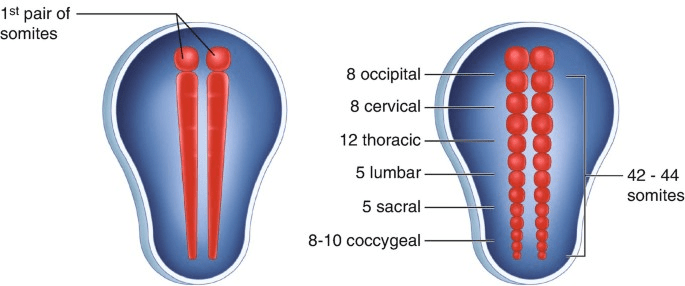
The somites then differentiate in a cranio-caudal direction into:
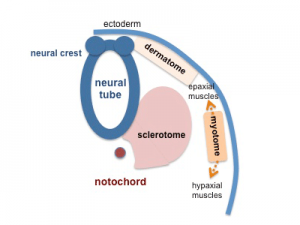
- Sclerotome – forms connective tissue, cartilage cells and bone cells of axial skeleton
- Myotomes – differentiate into myoblasts, which then forms skeletal muscles of the body
- Dermatome – forms dermis of skin
Intermediate mesoderm
- Cervical – segmented
- Thoracic – partially segmented
- Lumbar – unsegmented. forms nephrogenic cord (source of urinary system)
Origin to:
- Cortex of suprarenal gland
- Nephrons
- Gonads
Lateral plate mesoderm

Due to formation of intraembryonic coelom, it is divided into:
1. Somatic layer:
- Adherent to ectoderm
- Forms muscles and connective tissue of body wall
2. Splanchnic layer:
- Adherent to endoderm
- Forms serous membranes: Pleura, Pericardium, Peritoneum
- Smooth muscles
- Connective tissue of GIT, respiratory tracts
- Cardiovascular system
The intraembryonic coelom forms:
- Pericardial cavity
- Peritoneal cavity
- Pleural cavity
Other derivatives of the mesoderm:
- All skeletal, smooth and cardiac muscles
- Bone marrow and blood cells
- Spleen
- Lymph nodes
- Dura matter